Pneumoconiosis
Can I Get Social Security Disability Benefits for Pneumoconiosis?
- About Pneumoconiosis and Disability
- How to Get Disability Benefits for Pneumoconiosis by Meeting a Listing
- Residual Functional Capacity Assessment for Pneumoconiosis
- Getting Your Doctor’s Medical Opinion About What You Can Still Do
If you have pneumoconiosis, Social Security disability benefits may be available. To determine whether you are disabled by your pneumoconiosis, the Social Security Administration first considers whether it is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See How to Get Disability Benefits for Pneumoconiosis by Meeting a Listing. If you meet or equal a listing because of your pneumoconiosis, you are considered disabled. If your pneumoconiosis is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite the pneumoconiosis), to determine whether you qualify for disability benefits at Step 4 and Step 5 of the Sequential Evaluation Process.
About Pneumoconiosis and Disability
Pneumoconiosis is not a specific disorder, but rather refers to occupational interstitial fibrotic lung diseases caused by the inhalation of inorganic particle dusts like coal, beryllium, silicon and asbestos. Because pneumoconiosis involves fibrosis of the lungs themselves, it results in a parenchymal restrictive lung disease. Obstructive disease from bronchial reactivity may also be present, as well as obstructive disease as a co-existent disorder, e.g., emphysema caused by cigarette smoking. Also, infections such as tuberculosis may be present.
The development of pneumoconiosis usually requires long exposure over a period of years; in some instances, it may be 10–20 years before deterioration is severe enough to become prominent. Certainly, shorter exposures can produce disease and cause acute symptoms after heavy exposure. The major symptoms in the pneumoconioses are shortness of breath and cough; of course, easy fatigability would be associated with excessive exertion. The disease is irreversible. Cessation of exposure to the offending particulate dust is critical to slowing progression of the disease. To the extent that there is bronchoconstriction, bronchodilator drugs may improve air flow; antibiotics can be given for superimposed pneumonia; and supplemental oxygen in advanced cases as necessary. The possibility of malnutrition should always be considered in cases of significant pulmonary disease, and can easily be overlooked by the SSA. The most advanced cases of pneumoconiosis face death or lung transplantation. See Residual Functional Capacity Assessment for Pneumoconiosis.
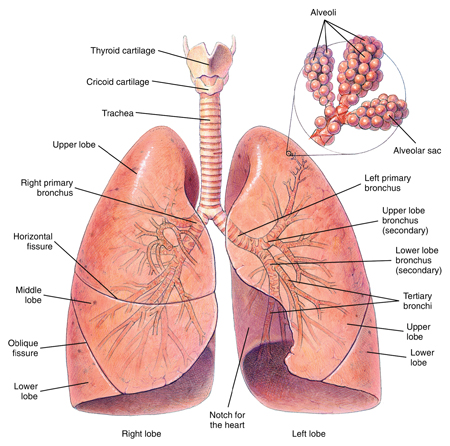
Respiratory System
Pneumoconiosis is caused by the inhalation of inorganic particle dusts like coal, beryllium, silicon and asbestos. These diseases include:
- Silicosis –Fibrotic lung disease resulting from inhalation of small particles of silicon dioxide (SIO2), which is the constituent of glass and sand. It is also a major component of many minerals and construction materials. The nodular form of silicosis is less likely to produce symptoms or functional limitations than the more severe conglomerate silicosis. In the latter, the pulmonary lesions are larger because of the coalescence of nodules; consequently the disorder is more serious. As in other forms of serious lung disease, patients with silicosis can have shortness of breath, cough, chest pain, loss of appetite, weight loss, malnutrition, sputum production, and exercise limitations. It is possible that lung lesions can compromise the arterial circulation in the lung, resulting in pulmonary hypertension which then leads to cor pulmonale (heart disease caused by lung disease) and right heart failure in extreme instances. Since several million workers are exposed yearly to silica, there is a significant public health burden and Social Security disability claims may arise from individuals who are inadequately protected at work. The mining industry is much more aware of silicosis and provides better safety to workers than manufacturing and construction industries where there is less of an awareness of the risk. Therefore, disabled claimants are more likely to come from these latter industries. It should be remembered that silicosis can occur in conjunction with other forms of pneumoconiosis.
- Berylliosis –A fairly rare lung disease, because of occupational safety regulations that limit exposure. Beryllium is a light metal element and is toxic in small amounts. Disease does not have to result from exposure to the pure metal: fumes or dust in the form of metal oxides, ceramic forms, and beryllium alloys can also result in lung damage. Pulmonary reactions are allergic in nature and acute exposures do not result in fibrotic lung disease. Acute disease is rapid in onset with pneumonia-like symptoms, while the chronic form leading to fibrotic lung damage is slowly progressive. The chronic form of berylliosis may involve fever, night sweats, loss of appetite, malnutrition (weight loss), cough, fatigue, and shortness of breath on exertion. There is an increased risk of lung cancer with berylliosis. Industries associated with occupations at risk include those in atomic energy, metal working, electronics, aerospace, mining, ceramics, and others. A test, known as the beryllium lymphocyte proliferation test (BeLPT), can help in identifying berylliosis. Possibly because of the relative rarity of berylliosis, the test is not widely available.
- Anthracosis (Black Lung Disease, Coal Workers’ Pneumoconiosis) –Fibrotic lung disease resulting from the chronic inhalation of coal dust. If the coal is mined where there is also a need to mine out hard rock with its high silica content, silicosis can complicate the anthracosis. Although anthracosis produces fibrotic lung disease, the obstructive lung diseases of emphysema and chronic bronchitis can also result from anthracosis. To determine the extent of contribution of anthracosis to emphysema is difficult, because of the high percentage of people with this disorder who smoke cigarettes and therefore have emphysematous and bronchitic components separate from the anthracosis. Although this fact may have some significance in personal injury litigation, it is only important in disability determination to be aware that both obstructive and restrictive deficits can be present and to determine their combined severity. Possible symptoms include fever, night sweats, loss of appetite, malnutrition (weight loss), cough, fatigue, and shortness of breath on exertion. However, the diagnosis of simple anthracosis does not automatically imply significant symptoms or functional limitations, but as small fibrotic nodules progress to larger masses, diffuse fibrosis of the lungs may be seen, along with emphysematous changes. Masses that put pressure on lung arteries can cause pulmonary hypertension with resultant cor pulmonale and heart failure.
- Asbestosis –Fibrotic lung disease caused by asbestos fiber inhalation, although the mechanism of disease induction is unknown. Despite knowledge of its danger in regard to fibrotic lung disease and cancer, asbestos remains a serious public health hazard. Not only are exposed workers at risk who handle asbestos-containing material, but others who might be secondarily exposed—such as family members exposed to asbestos fibers brought home on the clothing of the primarily exposed worker. As with other forms of pneumoconiosis, obstructive lung disease resulting from cigarette smoking may aggravate severity. In addition other abnormalities common to pneumoconiosis in general, asbestosis may produce distinctive abnormalities known as pleural plaques on a chest X ray. These plaques may be visible in the absence of other evident abnormality on the X ray, and thus can signal early disease before there is significantly limiting disease present. Collections of fluid may occur in the space between the inner chest wall and the lungs, a condition with a good prognosis is known as “benign asbestos-related pleural effusion,” and can be seen in the absence of other abnormalities.Possible symptoms are like those of similar mineral pneumoconioses: chest pain, cough, fever, night sweat, loss of appetite, weight loss, malnutrition, shortness of breath, exercise intolerance, and easy fatigability. It usually takes a long time, often more than 20 years, before disease manifests after exposure. The disorder is chronic and irreversible.
Other possible causes of pneumoconiosis include metal dusts (e.g., aluminum) or mineral dust forms of talc, tin, iron, mica, and kaolin. The important point is that chronic exposure to dust-like particulates that can be inhaled into the lungs may be conducive to restrictive lung disease and should be avoided regardless of the nature of the offending agent. Cigarette smoking is a major complicating factor that greatly increases severity.
Continue to How to Get Disability Benefits for Pneumoconiosis by Meeting a Listing.
