Hepatitis or Other Chronic Liver Diseases
Can I Get Social Security Disability Benefits for Hepatitis or Other Chronic Liver Diseases?
- How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Chronic Liver Disease?
- About Chronic Liver Disease and Disability
- Winning Social Security Disability Benefits for Liver Disease by Meeting a Listing
- Residual Functional Capacity Assessment for Chronic Liver Disease
- Getting Your Doctor’s Medical Opinion About What You Can Still Do
How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Chronic Liver Disease?
If you have any type of chronic liver disease, including chronic viral hepatitis, Social Security disability benefits may be available. To determine whether you are disabled by your chronic liver disease, the Social Security Administration first considers whether your liver disease is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Liver Disease by Meeting a Listing. If you meet or equal a listing because of chronic liver disease, you are considered disabled. If your liver disease is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your liver disease), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Liver Disease.
About Chronic Liver Disease and Disability
What Is Chronic Liver Disease?
Chronic liver disease is characterized by liver cell necrosis (death), inflammation, or scarring (fibrosis or cirrhosis) due to any cause that persists for more than 6 months.
Examples of Chronic Liver Disease
Examples of chronic liver disease include, but are not limited to:
- Chronic hepatitis;
- Alcoholic liver disease;
- Non-alcoholic steatohepatitis (NASH);
- Primary biliary cirrhosis (PBC);
- Primary sclerosing cholangitis (PSC);
- Autoimmune hepatitis;
- Hemochromatosis (liver damage from iron overload, resulting from a defect in the body’s ability to metabolize iron properly);
- Drug-induced liver disease;
- Wilson’s disease (a rare genetic disease caused by a defect in the body’s ability to metabolize copper); and
- Serum alpha-1 antitrypsin deficiency.
There are many other possible causes of liver disease, such as metabolic disorders (e.g., cystic fibrosis, porphyria, glycogen storage disease), vascular diseases (e.g., polymyalgia rheumatica, polyarteritis nodosa), parasitic infections (particularly roundworms, tapeworms, and flatworms), bacterial and fungal infections, toxins and drugs, and autoimmune hepatitis.
Some cases of liver failure are caused by an unknown agent.
Signs and Symptoms of Chronic Liver Disease
Signs of chronic liver disease may include:
- Jaundice (yellowing of the skin),
- Enlargement of the liver and spleen,
- Ascites (fluid in the abdomen),
- Peripheral edema (swelling of extremities), and
- Altered mental status.
Symptoms may include:
- Pruritis (itching),
- Fatigue,
- Nausea,
- Loss of appetite, or
- Sleep disturbances.
Symptoms of chronic liver disease may have a poor correlation with the severity of liver disease and functional ability.
Laboratory Findings Associated With Liver Disease
With liver disease, blood tests may show increased liver enzymes, increased serum total bilirubin, increased ammonia levels, decreased serum albumin, and abnormal coagulation studies, such as increased International Normalized Ratio (INR) or decreased platelet counts.
Abnormally low serum albumin or elevated INR levels indicate loss of liver function, with increased likelihood of cirrhosis and associated complications. However, other abnormal lab tests, such as liver enzymes, serum total bilirubin, or ammonia levels, may have a poor correlation with the severity of liver disease and functional ability.
A liver biopsy may demonstrate the degree of liver cell necrosis, inflammation, fibrosis, and cirrhosis. If you have had a liver biopsy, the Social Security Administration will make every reasonable effort to obtain the results; however, it will not pay for you to have one.
Imaging studies (CAT scan, ultrasound, MRI) may show the size and consistency (fatty liver, scarring) of the liver and document ascites (fluid in the abdomen).
Chronic Viral Hepatitis Infections
Hepatitis means inflammation of the liver. If lasting more than about 6 months, it may be termed chronic. Prolonged hepatitis can lead to cirrhosis.
Although there are several different types of viral hepatitis infections, chronic viral hepatitis infections are commonly caused by hepatitis C virus (HCV), and to a lesser extent, hepatitis B virus (HBV). Usually, these are slowly progressive disorders that persist over many years during which the symptoms and signs are typically nonspecific, intermittent, and mild (for example, fatigue, difficulty with concentration, or right upper quadrant pain).
The spectrum of these chronic viral hepatitis infections ranges widely. Some patients may have no symptoms; others may have only mild to moderate symptoms. Some may develop cirrhosis, end stage liver disease with the need for liver transplantation, or liver cancer.
Chronic Hepatitis B (HBV) Infection
Chronic HBV infection is diagnosed by the detection of hepatitis B surface antigen (HBsAg) in the blood for at least 6 months. The goal of treatment is to suppress HBV replication and thereby prevent progression to cirrhosis and end stage liver disease. Treatment usually includes a combination of interferon injections and oral antiviral agents.
The hepatitis B virus is a highly infectious organism. Worldwide, there are hundreds of millions of carriers. Millions of individuals die yearly from hepatitis B viral infections. HBV may induce a form of liver cancer known as hepatocellular carcinoma that kills many hundreds of thousands of people worldwide every year.
In the U.S., probably less than 1% of the population are carriers. This is much lower than in some other parts of the world where the majority of individuals have been infected. High-risk groups for infection are male homosexuals, IV drug users, and individuals working in healthcare who are exposed to blood or blood products.
There is about a 10% chance of infection of a person who suffers an accidental stick with a needle contaminated with the blood of a HBV carrier. Donated blood is routinely screened for hepatitis B to prevent transmission by transfusion, but this doesn’t protect health workers exposed to blood in the course of a patient’s care. In addition to blood, a carrier has virus in semen, saliva, vaginal secretions, sweat, tears, urine, and breast milk.
If swallowed, the virus is destroyed by pancreatic enzymes in the digestive tract which probably explains why oral transmission is rare and transmission in food has not been documented. In the rare cases of oral transmission, infection probably occurred because of breaks in the oral mucosa or gingiva that allowed the virus to directly enter the bloodstream.
Transmission of the virus from blood or other bodily fluids through small cuts or abrasions in the skin or mucous membranes of which a person is unaware may explain why as many as 50% of infected individuals have no history of high-risk exposure. As many as 80% to 90% of infected individuals are unaware they are carriers.
Maximum symptoms occur at about 3 to 5 months after initial infection and correspond to the greatest liver inflammation as reflected by a peak in transaminase liver enzymes. Once infected, some individuals may die within a matter of weeks from severe and aggressive hepatitis and liver failure, but this outcome involves less than 1% of cases. Most patients (90% to 95%) will have a full recovery, and 5% to 10% will become chronic carriers of the virus.
Carriers with no symptoms who also have normal levels of transaminase enzymes have a good prognosis, because they have no continuing hepatitis. Those who have abnormal transaminases indicative of continuing hepatitis have a poorer prognosis even if they have no symptoms. Such carriers are more likely to develop chronic persistent hepatitis (CPH), chronic active hepatitis (CAH), and hepatocellular carcinoma.
Chronic Hepatitis C (HCV) Infection
Chronic HCV infection is diagnosed by the detection of hepatitis C viral RNA in the blood for at least 6 months. Hepatitis C can be transmitted in blood and can cause both acute and chronic liver inflammation, as well as cirrhosis of the liver. Along with alcohol abuse, hepatitis C is the most common cause of cirrhosis. At least 4 million people in the U.S. are infected, and many are unaware that they are infectious. Risk of infection is increased by sexual intercourse with infected individuals and by intravenous drug use. About half of infected individuals progress to chronic active hepatitis (CAH) and have an associated increased risk of liver cancer.
Treatment usually includes a combination of interferon injections and oral ribavirin. Whether a therapeutic response has occurred is usually assessed after 12 weeks of treatment by checking the HCV viral load. A substantial reduction in HCV viral load (also known as early viral response, or EVR) predicts a sustained viral response with completion of treatment. Combined therapy is commonly discontinued after 12 weeks when there is no early viral response, since in that circumstance there is little chance of obtaining a sustained viral response (SVR). Otherwise, treatment is usually continued for a total of 48 weeks.
Combined interferon and ribavirin treatment may have significant adverse effects that may require dosing reduction, planned interruption of treatment, or discontinuation of treatment. Adverse effects may include: anemia (ribavirin-induced hemolysis), neutropenia (low neutrophil [type of white blood cell] count), thrombocytopenia (low platelet count), fever, cough, fatigue, myalgia (muscle pain), arthralgia (joint pain), nausea, loss of appetite, pruritis (itching), and insomnia. Behavioral side effects may also occur. Influenza-like symptoms are generally worse in the first 4 to 6 hours after each interferon injection and during the first weeks of treatment. Adverse effects generally end within a few days after treatment is discontinued.
Chronic Active Hepatitis
Chronic active (aggressive) hepatitis (CAH) is a very serious disorder whose specific cause is unknown, but may involve some abnormal immune response by the liver to a particular agent. If the CAH is related to intake of a drug, it may rapidly improve with withdrawal of that drug. However, cases associated with viral infections have a much poorer prognosis. Overall, CAH has a high mortality despite treatment, and sometimes can be associated with problems in organ systems other than the liver. These include arthralgia (joint pains), anemia, fibrosis of the lungs, intestinal inflammation, and kidney disease.
Cirrhosis
The most frequent kind seen by the Social Security Administration is cirrhosis of the liver caused by the abuse of alcohol. The term cirrhosis refers to present or past evidence of hepatic (liver) cell necrosis (death), fibrosis (replacement of normal cells with fibrous tissue), and areas of regenerating nodules of liver tissue attempting to recover from previous damage.
Tissue for microscopic evaluation must be removed from the liver (biopsy), which is the only way a certain diagnosis of cirrhosis can be made. The Social Security Administration does not purchase liver biopsies on claimants. When they are done by a treating source, they are usually percutaneous—a needle is inserted into the liver through the skin between the right lower ribs under local anesthesia and can be done at the bedside.
The liver makes and secretes bile into the bile ducts, and these ducts in turn carry bile to the gallbladder for storage, and also to the small intestine (see Figure 1 below). Bile assists in the absorption of fats from the intestine. Biliary cirrhosis results when normal bile flow is interrupted and the liver cells are exposed to it. Primary biliary cirrhosis is usually found in older females and involves obstruction to bile flow in the small biliary ducts inside the liver itself. Secondary biliary cirrhosis involves obstruction of the larger ducts outside the liver (extrahepatic ducts) with a consequent back-pressure of bile into the liver. Gallstones may produce an obstruction, or stricture related to previous surgery, or rarely an obstructing cancer.
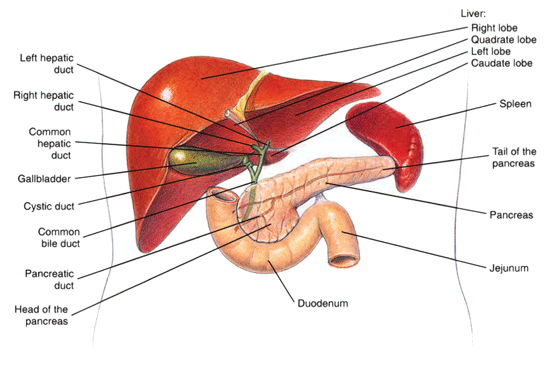
Figure 1: The liver, pancreas, and duodenum.
Toxins as a Cause of Hepatitis
Many toxic substances can cause hepatitis, the most prominent of which is excessive alcohol intake. People vary greatly in the efficiency with which their liver can metabolize alcohol, and there is no way to predict individual capacity in this regard. By far, alcoholic hepatitis is the most frequent form of hepatitis and is usually acutely superimposed upon a more chronic underlying cirrhosis. As a patient is detoxified in a treatment facility, the alcoholic hepatitis improves with progression of residual chronic cirrhosis. Some cases of acute alcoholic hepatitis are fatal and cirrhosis eventually results in the death in many others.
Acute Hepatitis
Alcoholics, in particular those who have been binge drinking, can have an episode of acute alcoholic hepatitis superimposed on an underlying chronic liver disease. When hospitalized where alcohol is unavailable and treated, the acute hepatitis can improve. In these claims, the Social Security Administration can be expected to hold the claim for a few months to determine what degree of improvement will occur with treatment of the acute episode.
Claimants with acute viral hepatitis will be treated similarly, because most will improve over the short term.
Continue to Winning Social Security Disability Benefits for Liver Disease by Meeting a Listing.
