Can I Get Social Security Disability Benefits for Schizophrenia?
- How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Schizophrenia?
- About Schizophrenia and Disability
- Winning Social Security Disability Benefits for Schizophrenia by Meeting a Listing
- Residual Functional Capacity Assessment for Schizophrenia
- Getting Your Doctor’s Medical Opinion About What You Can Still Do
How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Schizophrenia?
If you have schizophrenia, Social Security disability benefits may be available. To determine whether you are disabled by schizophrenia, the Social Security Administration first considers whether the schizophrenia is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Schizophrenia by Meeting a Listing. If your schizophrenia is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite schizophrenia), to determine whether you qualify for disability benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Schizophrenia.
About Schizophrenia and Disability
What Is Schizophrenia?
Schizophrenia is a serious mental disorder for which there is no cure. Schizophrenia affects about 1% of the adult population. There are various types of schizophrenia, i.e., disorganized, catatonic, residual, undifferentiated, and paranoid. Any of these forms of schizophrenia may entitle a person to disability benefits.
Schizophrenia appears before age 45, usually in the adolescent or young adult. The person exhibits a definite deterioration from a previous level of functioning in social, work, and personal life. Psychological abnormalities are diverse, affecting:
- Thought.
- Perception.
- Emotion (affect).
- Identity.
- Ability to plan and carry out purposeful activity.
- Cognition (ability to think, learn, and understand).
- Sociability. The person may experience a tendency to withdraw from the outside world and a preoccupation with illogical ideas, fantasies, or delusions.
- Movement. The person may exhibit a decrease, increase, or bizarreness of movements or postures.
The prevailing view of schizophrenia has been that the psychotic features are the most important and that cognitive deficits are secondary. However, the latest research suggests that the cognitive deficits, which arise from various brain abnormalities, are the more fundamental cause of mental abnormalities in schizophrenia. In fact, there is reason to think that subtle brain abnormalities appear before a child is born and gradually increase in severity.
Causes of Schizophrenia
The disorder involves biochemical dysfunction in the brain, but no one can as yet describe the mechanisms involved. Numerous abnormalities are found in the brains of those with schizophrenia (see Figures 2 and 4 below).
There is also a complex genetic predisposition that no one is close to understanding. It is thought that about 40% of cases of schizophrenia are inherited, and 60% occur spontaneously. Recent research suggests that schizophrenia may result from a large number of genetic abnormalities (see Figures 1 and 3 below). Consequently, there is no chance of a single cause and cure for schizophrenia.
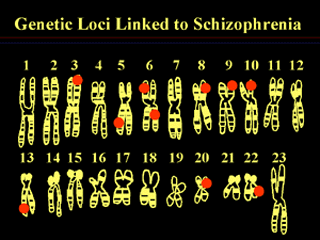
Figure 1: A so-called “linkage study,” showing a number of places in the human genome where pieces of DNA are inherited along with risk for the illness. It shows one of each of the 23 pairs of chromosomes, and the red dots indicate regions where a piece of DNA has been shown to be inherited along with the risk for schizophrenia in certain families and certain studies.
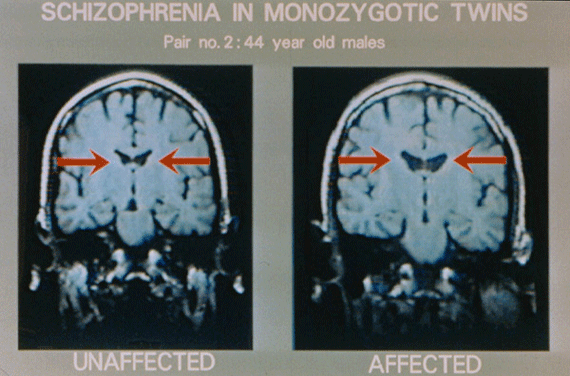
Figure 2: MRI scans of identical twins. The twin on the right has schizophrenia; the twin on the left is healthy. Even to the unprofessional eye, there are obvious differences, a systematic and consistent variation between the affected and the unaffected twin in the gross anatomy of the brain. Red arrows point to enlarged ventricles in the affected twin.
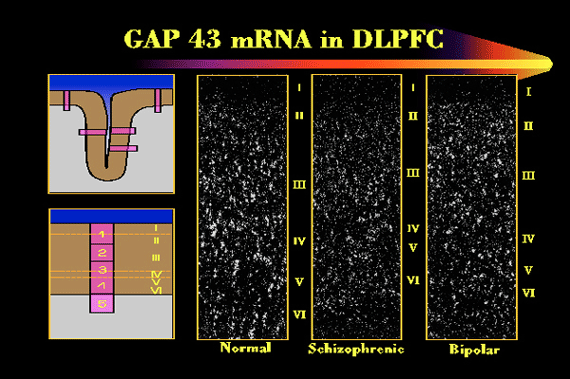
Figure 3: Each white dot represents cells in a particular part of the brain. A patient with schizophrenia is compared to an individual with another psychiatric illness, bipolar disorder, and to a normal subject. The white dots show the turning-on of a gene that is the blueprint for a protein related to the process by which cells adapt themselves to a changing environment. I–VI represent layers of the cerebral cortex.
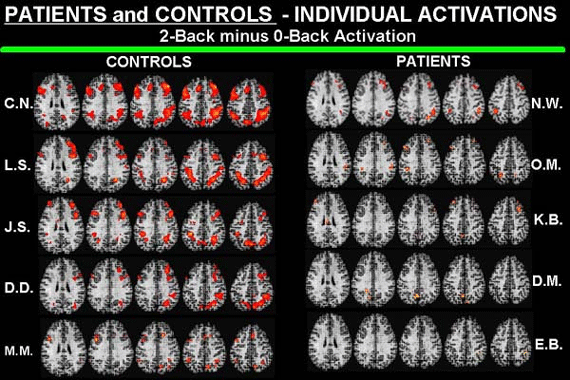
Figure 4: PET scans of five normal individuals (left); each row is one person, and each image is a slice from five different levels of the person’s brain. The red areas show regions of the brain that are activated when a person performs a memory task. In PET scans of five individuals with schizophrenia (right), each row represents a different person, with comparable slices. Clearly, the patients with schizophrenia do not generate the dramatic brain activity in the circuits of the brain critical to the memory task.
Phases of Schizophrenia
Schizophrenia usually has 3 phases.
- First, there is the prodromal phase. The duration of this phase is variable. The person shows a clear deterioration from the previous level of functioning in multiple areas of life—mental, occupational, personal, and social. The “change in personality” is often noticed by friends and relatives, as the person withdraws from usual activities, engages in less effective and increasingly strange behavior and experiences difficulty with clear and logical communication with others.
- Next is the active or progressive phase. In this phase, overt psychotic symptoms become obvious. The impairments present in the prodromal phase become more severe. The individual increasingly withdraws. Strange behavior may become bizarre or completely disorganized, and odd perceptions and thought develop into hallucinations and delusions. Abnormalities in the form and content of thought produce further confusion and difficulty communicating with others. Transition from the prodromal to the active phase is often triggered by stress that the person cannot cope with. For example, such a stressor might be a serious physical illness or change in an important relationship with another person. Or it might be something that a normal person would consider trivial.
- A residual phase follows the active phase. Psychotic symptoms persist to some degree, but the accompanying emotions are not as intense. (The residual phase should not be confused with the residual type of schizophrenia, so-called because an active, florid phase of the illness is missing.) Unfortunately, normal emotional responsiveness tends to be subdued also. Residual functional impairment may remain severe.
The majority of claimants seeking disability benefits for schizophrenia are in the residual phase, and in some degree of remission on neuroleptic drugs which must be taken indefinitely. However, schizophrenia almost never goes into complete remission.
Cognitive Impairment With Schizophrenia
It is very important for the Social Security Administration to pay attention to cognitive dysfunction when assessing whether a person with schizophrenia is disabled. The Social Security Administration and many psychiatrists and psychologists still emphasize the psychotic features (hallucination, delusions) of the disease. So if a claimant’s psychotic features are controlled by medication, the Social Security Administration is not likely to test memory or other cognitive functions. Fewer than 10% of patients with schizophrenia ever get a regular job or live independently. At least 90% of people with schizophrenia are apparently incapable of working on any sustained basis.
Side Effects of Schizophrenia Medications
The drugs taken to lessen the symptoms of schizophrenia can cause side effects. The severity varies from person to person. In the early phase of drug therapy, symptoms may include muscle spasms, tremors, dry mouth, drowsiness, blurry vision, and restlessness. Changing the type of medication or the dosage can help control these symptoms.
Older medications were associated with a risk of the patient developing tardive dyskinesia—a disorder characterized by involuntary movements, especially of the lips, tongue, and mouth. Newer medications, such as clozapine (Clozaril), olanzapine (Zyprexa), quetiapine (Seroquel) and resperidone (Resperdal) are associated with other risks. For example, clozapine can cause a decrease in white blood cells and greatly weaken the body’s defense against dangerous infections. Clozapine can also cause seizures, inflammation of the heart (myocarditis), low blood pressure (hypotension), and other side effects. Olanzapine (Zyprexa) can cause weight gain and Parkinsonian movement disorders. Anyone taking antipsychotic medications must be monitored by a doctor.
If the claimant is having medication side-effects, a Social Security Administration psychiatrist or other medical doctor, rather than a Social Security Administration psychologist, should evaluate at least that part of the claim.
Information from Family and Friends Is Crucial to Disability Determination
Claimants with chronic schizophrenia living with family members are most likely to be improperly denied Social Security disability benefits. It is critically important for family members or other caregivers to provide the Social Security Administration with as detailed information as possible about specific tasks the claimant can or cannot do.
Mental health clinics will often refuse to provide the Social Security Administration with clinical records that are useful in evaluating how a mental disorder has developed over time. They might simply write a letter summarizing what they think they Social Security Administration needs to know. In some instances, the Social Security Administration is forced to fall back on purchasing a consultative mental status examination in which the examining psychiatrist or psychologist has limited time to determine the details of daily functional capacity. The Social Security Administration should ask the treating psychiatrist (or psychologist) about work-related abilities for at least unskilled work and how these conclusions match with the corresponding limiting mental symptom.
If the claimant is receiving medication, information about side-effects must come from a medical doctor, because a psychologist is not competent to evaluate that matter. However, it is also important for the same kind of information and opinions to be obtained from family or other caregivers, to make sure that nothing is missed. The caregivers live with the claimant; they may have noticed important facts that can be brought to the treating psychiatrist’s attention and to the Social Security Administration.
Continue to Winning Social Security Disability Benefits for Schizophrenia by Meeting a Listing.
