Chronic Persistent Lung Infections
How to Get Disability Benefits for Chronic Persistent Lung Infections by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your chronic persistent lung infection is severe enough to meet or equal the chronic persistent listing. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that Social Security Administration presumes would prevent a person from performing substantial work. If your chronic persistent lung infection is severe enough to meet or equal the listing, you will be considered disabled.
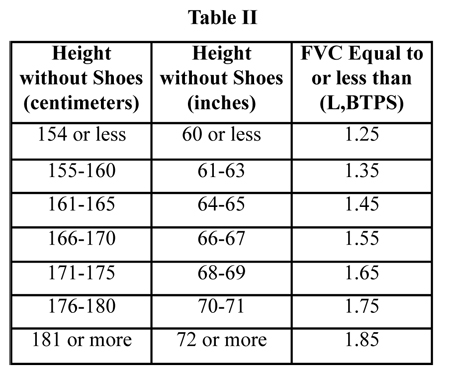
The listing for chronic persistent lung infections is listing 3.08. Generally, to meet the listing, you must have a chronic persistent lung infection that results in limitations in pulmonary function. Your forced vital capacity (FVC) reported in pulmonary function testing must be equal to or less than the values specified in Table II below (corresponding to the person’s height without shoes):
Chronic Pulmonary Insufficiency
However, listing 3.08 also says, “In those unusual cases of pulmonary infection that persist for a period approaching 12 consecutive months, the clinical findings, complications, therapeutic considerations, and prognosis must be carefully assessed to determine whether, despite relatively well-maintained pulmonary function, the individual nevertheless has an impairment that is expected to last for at least 12 consecutive months and prevent gainful activity.”
Chronic Persistent Lung Infections and Pulmonary Function Testing.
In practice, the SSA does not often see TB advanced enough to seriously compromise breathing in non-immunocompromised claimants. In claimants with advanced active lung infection either from mycobacteria or mycoses fungi, allowance would probably be possible by a combination of factors without pulmonary function tests. In any event, spirometry is not advised if you have an active and contagious pulmonary infection, because of the danger of infecting other people being tested using the same equipment until control of the infection is achieved. Pulmonary specialists have been able to prevent transmission of infectious agents like TB through spirometers by installing special filters in the equipment and changing mouthpieces between patients. It is presumed that the filters are fine enough to capture bacteria such as TB, fungi, and even potentially lethal viruses like HIV. To date, there is no reason to doubt this conclusion. Many non-pulmonary specialist private physicians performing spirometry for the SSA do not have the expertise to safety handle spirometric testing of individuals with contagious pulmonary infections. In any event, spirometry done in the presence of acute pulmonary infection would be invalid for allowance of benefits, since it may not represent optimal performance. In chronic infection, the situation is different because duration is no longer an issue.
In the case of TB, if spirometry must be done by the SSA, the proper procedure is wait until cultures are negative for the growth of TB bacteria. If chronic lung damage, e.g., from cavitation and/or fibrosis, is extensive enough then a restrictive deficit as evidenced by a decline in the forced vital capacity (FVC) might be evident. In real life, those claimants who have uncontrolled TB are also likely to be smokers with resultant chronic obstructive lung disease (COPD) with a decline in the forced expiratory volume in the first second (FEV1) of expiration.
It should be realized that TB and fungal infections can occur together (a weakened immune system that allows one type of infection to progress also may provide an opportunity for other infections). As noted above, smoking may impose further impairment so that the severity of three or more pulmonary disorders have to be considered in the same claimant.
Continue to Residual Functional Capacity Assessment for Chronic Persistent Lung Infections.
Go back to About Chronic Persistent Lung Infections and Disability.
